Detecting and dealing with low mood as a secondary problem
One of the earliest CBT skills that I frequently find myself teaching clients is how to detect and deal with a mood that has become secondarily lowered by their main problems.
Clearly, it isn’t just those who satisfy a DSM diagnosis of depression who have low mood, but also often those suffering with any one of the anxiety disorders. It’s usually apparent in the assessment sessions if the client has a lowered mood: her baseline PHQ-9 measure may suggest lowered mood; she may explicitly state she feels low or sad or her thoughts and behaviours may contain content pertaining to loss or withdrawal.
If so, I usually suggest the client undertakes a Mood Diary for the first or second session homework. I use a simple 5 column Diary with the headings as follows:
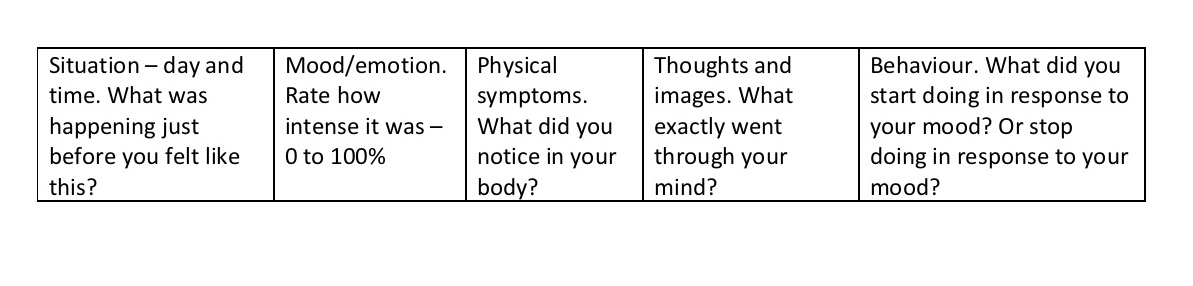 Mood Diary
Mood Diary
I take care to explain how to use the Diary during the session, especially the ‘feelings take one word to describe’ rule. Most clients conflate emotions with thoughts and it’s helpful to get this right from the outset by explaining that reporting thoughts usually require a sentence while feelings require a word. It’s worth advising the client to only document emotions that are intense enough to cause significant distress, say 50% or more than the strongest possible such emotion. (I have received a three page dossier of 20% this and 15% that before now…)
In the next session, we will obviously review the diary. The commonly occurring depressive emotions include feeling sad, bleak, alone, hopeless, worthless, small, bad, guilty, like a burden, inadequate, lazy, bad etc. Emotions relating to the client’s main diagnosis will also be documented, such as those indicative of anxiety or panic etc.
I use the following micro-formulation to show the client the relationship between low mood and worry very clearly. I find this micro-formulation totally invaluable and use it constantly, making it one of my most prized golden nuggets.
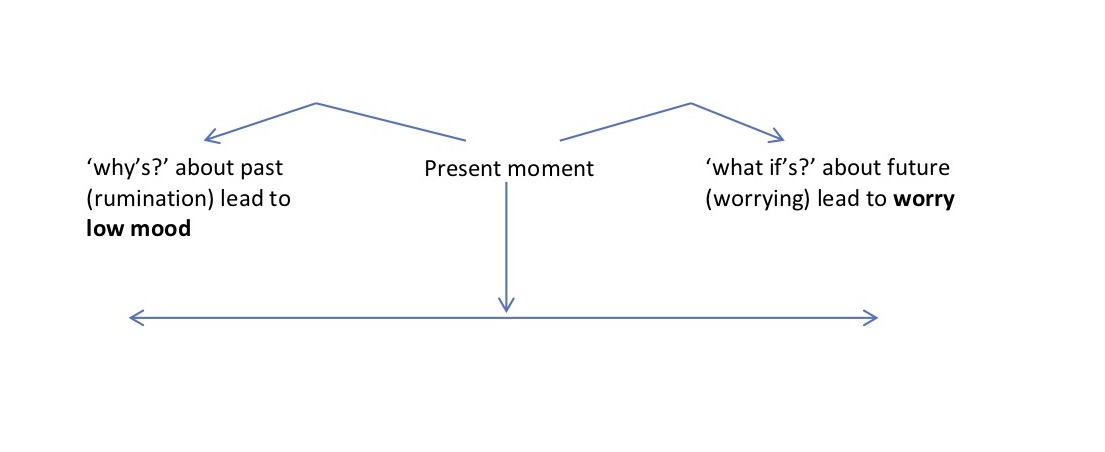
Micro-formulation linking low mood and worrying
This micro-formulation helps the client who comes in saying ‘I have anxiety’, understand why she also has a lowered mood. It also helps the client who comes in saying ‘I’m depressed’, understand why she often also feels anxious.
You may have detected my deliberate use of the symptoms terms ‘low mood’ and ‘worry’ rather than the diagnostic terms ‘depression’ and ‘anxiety’. This is because some clients feel even worse if they’ve come in expecting to get one diagnosis and then feel like they’ve ended up being given two! Sticking to describing symptoms in this instance can feel less threatening and more manageable.
The micro-formulation also shows how the problematic behaviours of ruminating and worrying maintain the low mood/depression and the worry/anxiety. This identification of rumination and worrying as maintaining processes links us back into the formulation and indicates that we have to target these behaviours in order to make the client feel better.
Having identified the contribution of low mood to the client’s distress, I may now suggest undertaking one week of activity monitoring and scheduling as an early intervention to lift mood. For a client in whom low mood is a secondary, contributory but not the major problem, I explain the activity monitoring and scheduling as follows:
‘We’ve seen how your mood is becoming low because you’re naturally tending to dwell on your problems. People with low mood often find that life becomes gradually less pleasurable and rewarding, even if they don’t notice this is happening, and even if they’re actually busy and actually getting most things done at work and at home as usual. It might be valuable to see if this is happening with you to any extent. Here is an activity diary to complete for the first few days of the week…’
and I show her how to complete the diary. I use the planner available at
https://www.getselfhelp.co.uk/docs/WeeklyPlanner.pdf
‘In the first few days, you could note down what activities you usually do and then rate how much pleasure or sense of reward they give you. Midweek, you could switch to scheduling in a couple of small things daily that you know you enjoy or find rewarding. They don’t have to be big activities, just simple, everyday pleasures. What kind of thing could that be for you? So you need to deliberately schedule those things in, by time-slot and in advance, otherwise it’s easy to forget to do them! Once you’ve done them, it’s important to re-rate your mood as before.’
If the debriefing of this homework in the following session shows a slight lifting of mood, I recap the micro-formulation and ask how the client thinks she can take the learning forward into coming weeks.
Clearly this rather didactic and concise approach is not suitable for clients who are severely depressed –they will require a much more in-depth and systematic approach, perhaps using Behavioural Activation and definitely by unpacking their negative automatic thoughts etc. But it can be a quick, pick-me-up technique for some and one that I find useful.
Summary points
2. Use a simple Mood Diary to monitor suspected low mood as an early homework
3. Micro-formulate the link between low mood and worrying
4. Be sensitive to using the terms ‘depression’ and ‘anxiety’ early on, before the client has had the opportunity to learn coping skills
With thanks to Lee Grant at Efficiacy, from whom I first learned this particular micro-formulation.







